Why a Biopsy Is Needed for Lung Cancer Diagnosis
If you have had a chest X-ray or CT scan that looks suspicious, it’s completely normal to think, “So that’s it then. That proves it.”


Jump to:
- What a biopsy actually tells us
- Why scans are not enough on their own
- The biopsy’s second job: guiding the right treatment
- 1) Staging needs confirmation, not assumptions
- 2) Modern treatment depends on tumour biology
- 3) Sample quality matters more than people realise
- How we choose the best type of biopsy
- Common biopsy methods for suspected lung cancer
- Bronchoscopy
- EBUS biopsy (lymph node sampling)
- CT-guided needle biopsy (through the skin)
- Pleural fluid sampling and pleural biopsy
- Surgical biopsy
- Preparing for a biopsy and what recovery looks like
- How long do results take?
- Common questions patients ask
- From Uncertainty to a Clear Treatment Path
- About Dr James Wilson
While scans might strongly suggest lung cancer - they aren’t able to make the diagnosis. There are other things that can look like lung cancer on a scan that need different treatment.
A biopsy is how we make sure. It is the step where we take a small sample of tissue or cells, look at it under the microscope, and work out exactly what we are dealing with. Not just whether it is cancer, but what kind of cancer, and what treatment is most likely to help.
What a biopsy actually tells us
A biopsy does three very practical things.
First, it confirms whether it is cancer. Plenty of conditions can look worrying on a scan. Infection, inflammation, scarring, and benign growths can all mimic cancer radiologically. Imaging is brilliant, but it does not identify cells.
Second, it tells your oncology consultant what type of lung cancer it is. Broadly, we separate lung cancer into small cell and non-small cell. Within non-small cell, the subtype matters, too. Treatment decisions change depending on what the pathologist sees.
Third, it gives us information that helps with staging and treatment planning. In other words, it helps us move from “there’s something there” to “here’s the plan”.
Why scans are not enough on their own
CT and PET-CT (Positron Emission Tomography-Computed Tomography) scans give us a detailed map. They show size, location, lymph nodes that look involved, and whether there are signs of disease elsewhere.
But scans cannot answer the question patients actually care about, which is, “What is it, exactly?”
PET-CT scans can light up areas that are not cancer. Inflammation can do that. Infection can do that. Even normal tissues can show activity. So while PET-CT is extremely useful for assessing spread, I feel that it is not a substitute for tissue confirmation.
That is why, in most cases, the lung cancer diagnosis is not considered secure until we have a biopsy result.
The biopsy’s second job: guiding the right treatment
Once we have tissue, we can do more than confirm “yes or no”.
1) Staging needs confirmation, not assumptions
Lung cancer staging is often described using the TNM system. It is a way of describing the tumour itself (T), whether lymph nodes are involved (N), and whether there is metastasis or spread elsewhere (M).
Here’s why that matters: If a lymph node looks suspicious on a scan, it might be cancer. Or it might be reactive, for example, due to inflammation. A biopsy of lymph nodes can make the difference between a treatment plan aimed at a cure and one aimed at control. That is not a small detail.
2) Modern treatment depends on tumour biology
For many patients with non-small cell lung cancer, the biopsy sample is also used for molecular and biomarker testing.
This looks for changes in the tumour that can predict which treatments are more likely to work, including targeted therapies and immunotherapy. The key point is simple. We cannot personalise treatment without the right material to test.
3) Sample quality matters more than people realise
Sometimes a biopsy confirms cancer, but the sample is too small to run all the tests we need. That can lead to a repeat procedure.
This is perhaps one of the most frustrating parts of the pathway for patients. It feels like a delay. Clinically, though, it is usually about getting enough high-quality tissue to do the job properly, including the additional testing that guides treatment.
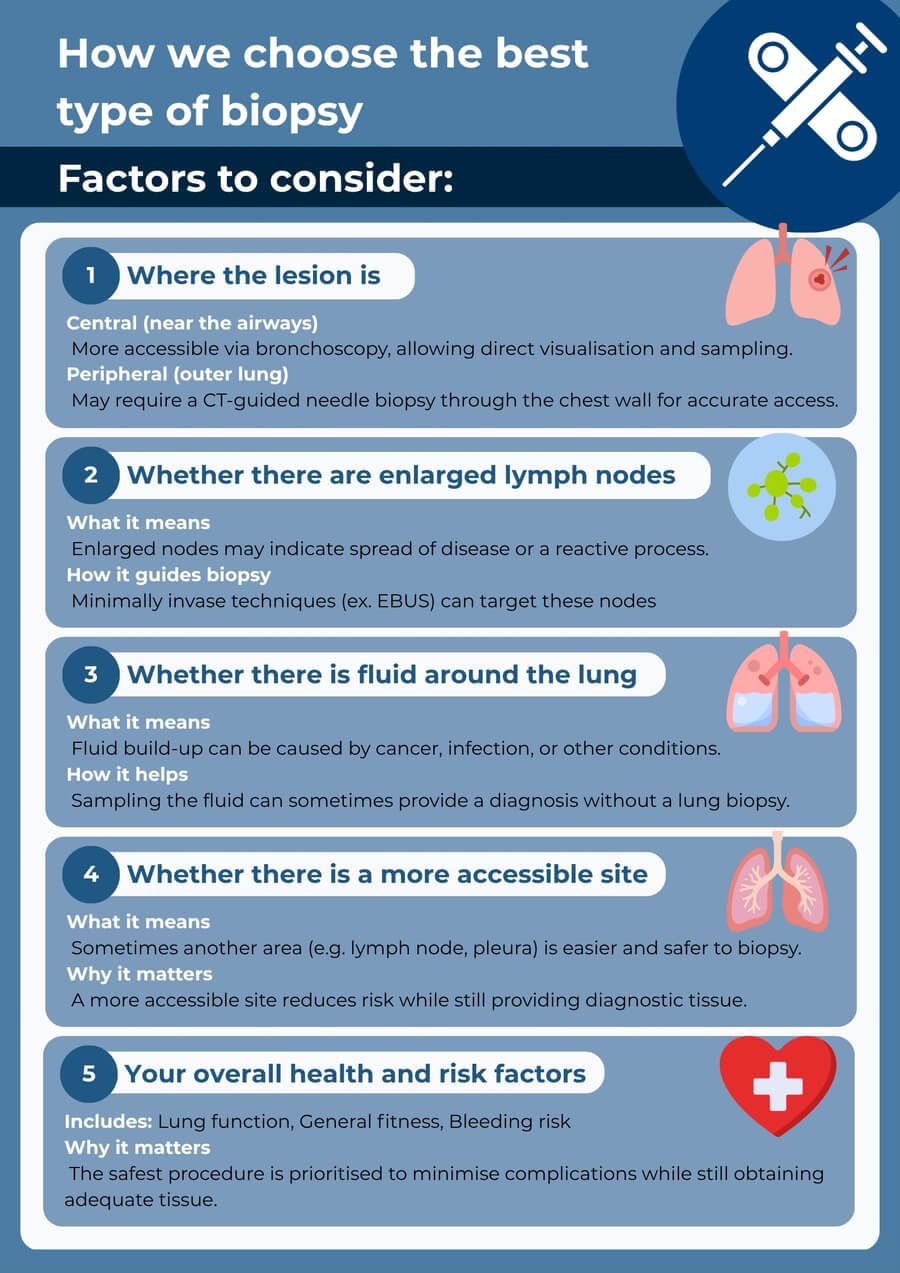
How we choose the best type of biopsy
There is no one biopsy solution for all conditions. We choose the approach based on what is safest and most likely to give a clear answer.
Factors include:
- Where the lesion is (central near the airways vs more peripheral)
- Whether there are enlarged lymph nodes
- Whether there is fluid around the lung (pleural effusion)
- Whether there is a more accessible site to sample
- Your overall health, lung function, and bleeding risk
Common biopsy methods for suspected lung cancer
Bronchoscopy
A bronchoscopy uses a thin flexible camera passed through the nose or mouth into the airways. It is particularly useful if the abnormality is close to the larger airways.
It’s usually done with local anaesthetic and sedation. People often feel a sore throat afterwards, and it’s fairly common to experience a little bit of coughing after this procedure.
EBUS biopsy (lymph node sampling)
EBUS stands for endobronchial ultrasound. It is a bronchoscopy combined with ultrasound guidance, allowing us to sample lymph nodes with a needle in real time.
This is often used when staging is the main question, or when lymph nodes are the best target to confirm diagnosis.
CT-guided needle biopsy (through the skin)
If the nodule is in the outer parts of the lung, a CT-guided biopsy is often the most direct route. Local anaesthetic is used, and the radiologist guides a needle into the target area using imaging.
The main risk we discuss is pneumothorax, which is when air leaks and part of the lung collapses. Many pneumothoraces are small and settle with observation, but some require a chest drain. Bleeding can also occur, including coughing up a small amount of blood.
Afterwards, you are monitored for a few hours and usually have a chest X-ray to check if things look stable.
Pleural fluid sampling and pleural biopsy
If there is fluid in the lung, we may take a sample of that fluid. Sometimes a pleural biopsy is needed as well, depending on what we are trying to confirm.
Surgical biopsy
If less invasive methods are not possible or have not given a clear answer, a surgical approach may be recommended. This might involve sampling lymph nodes or taking a wedge of tissue, usually under general anaesthetic.
It’s more invasive, but it can provide larger tissue samples, which is sometimes exactly what we need.
Preparing for a biopsy and what recovery looks like
Preparation depends on the procedure, but a few themes are common.
- Blood thinners and antiplatelet medicines: You may need to stop these beforehand. This should always be done with clear medical guidance. Please do not stop them on your own.
- Fasting: If sedation or a general anaesthetic is planned, you will usually be asked not to eat or drink for a set period beforehand.
- Consent and risks: You should have a clear explanation of the benefits of the test and the risks, including pneumothorax, bleeding and, infection.
After the biopsy:
- You are usually observed for a period, particularly after a lung needle biopsy.
- Mild pain or discomfort is common. A small amount of blood in the sputum can happen after some procedures.
- You should be told what to watch for. Worsening breathlessness, chest pain, heavy bleeding, or fever should be treated seriously and assessed promptly.
How long do results take?
The initial pathology result often arrives within one week, depending on the lab and the complexity of the case.
Additional testing, including molecular profiling, can take additional time. This is another reason we aim to get a good sample at the first attempt. It reduces the risk of delays later.
Common questions patients ask
Can we start treatment for lung cancer without a biopsy?
Occasionally, yes, but I certainly advise against it. Most of the time, we need tissue confirmation to avoid treating the wrong condition and to choose the most effective treatment. We might sometimes talk to you about a liquid biopsy if getting tissue is challenging.
What if the biopsy is negative but the scan still looks suspicious?
A negative biopsy does not always mean “no cancer”. Sometimes the needle or forceps simply did not capture the right area. Your team may recommend a repeat biopsy or a different technique.
Will a biopsy make the cancer spread?
This is a common worry. In real-world practice, biopsies are routine and are performed because the benefit of accurate diagnosis and treatment planning overwhelmingly outweighs this concern.
Which biopsy is safest?
The safest biopsy is the one with the lowest risk that answers your situation. That is why the approach varies from person to person.
From Uncertainty to a Clear Treatment Path
A biopsy can feel like an added hurdle when all you want are fast, clear answers. But in most cases, it’s the step that transforms suspicion into certainty and replaces guesswork with a solid, actionable plan.
Without a biopsy, doctors are often working with incomplete information. Imaging can suggest what’s happening, but it can’t confirm the exact type of cancer or reveal the molecular details that now guide modern treatments. A biopsy provides that clarity, helping ensure that every decision moving forward is based on precise, reliable data.
If we’re going to treat lung cancer effectively, it has to be done with intention: the right diagnosis, at the right stage, using the right therapies. A biopsy is what makes that level of precision possible, and ultimately gives patients the best chance at a well-informed, personalised treatment plan.
About Dr James Wilson
Dr. James Wilson is a consultant oncologist with a focus on lung cancer and advanced radiotherapy. Practising full-time in Central London, he helps patients receive timely diagnoses, personalised treatment plans, and expert care when every moment counts.