When Lung Cancer Spreads to the Abdomen: Symptoms to Watch For
If you have lung cancer and develop symptoms in the tummy area (the abdomen), it’s easy to assume the worst. Most people do. To be honest, our brains favour speed over subtlety when we’re stressed.


Jump to:
- What does “spread to the abdomen” mean?
- The general symptoms worth reporting
- Symptoms by common site of spread
- Liver
- Adrenal glands
- Peritoneum and fluid build-up (ascites)
- Abdominal lymph nodes
- Bowel involvement (rare, but important)
- Pancreas (uncommon)
- Bone spread that feels like abdominal pain
- Common causes that are not cancer spread but still need treatment
- When to seek urgent help
- How we investigate abdominal symptoms
- What treatment and symptom relief can look like
- What you can do at home (without becoming your own full-time clinician)
- Doing the sensible thing
- About Dr. James Wilson
The truth is actually more boring. Abdominal symptoms are common, and in many cases, they are caused by things like constipation, reflux, infection, anxiety, or treatment side effects. That said, lung cancer can spread to parts of the abdomen, and when it does, it’s worth spotting symptoms early so we can intervene before they affect quality of life.
This guide covers what “spread to the abdomen” actually means, the symptoms that matter, what else can mimic them, and when to seek help.
What does “spread to the abdomen” mean?
When we say cancer has “spread”, we mean it has moved from the original tumour to another site through the bloodstream or lymphatic system. In lung cancer, “the abdomen,” or tummy, usually refers to a few specific areas:
-
Liver
-
Adrenal glands (they sit above the kidneys; they are often included in staging scans)
-
Abdominal lymph nodes
-
The lining of the abdomen (peritoneum), which can lead to fluid build-up (ascites)
-
Less commonly, the bowel, pancreas, or other abdominal organs
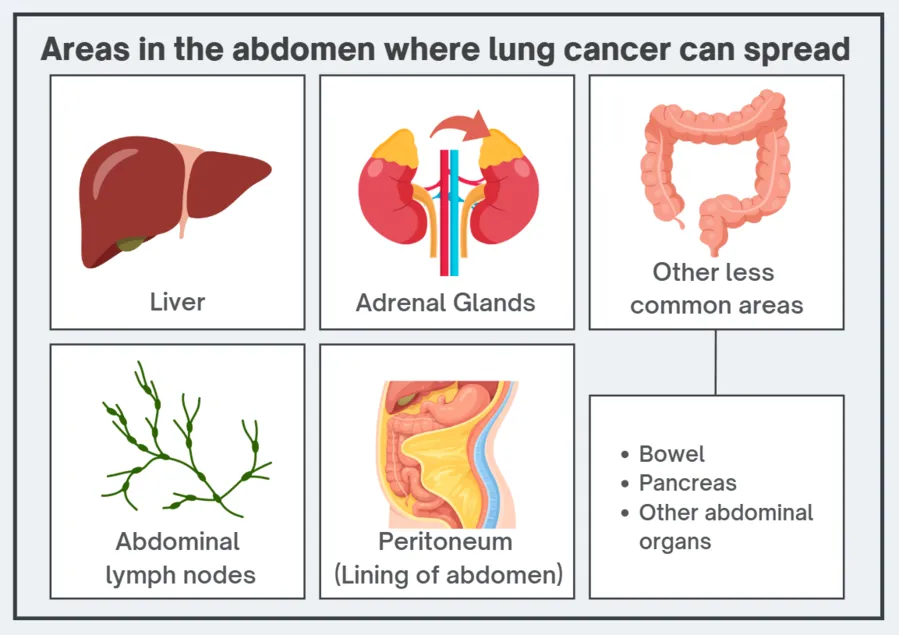
One important point to remember: Spread to the abdomen is often found on scans before it causes obvious symptoms. Symptoms can help, but they are not a reliable “map”.
The general symptoms worth reporting
These symptoms are not specific to cancer spread. But if they are new, persistent, or clearly worsening, they deserve attention:
-
Ongoing abdominal pain or pressure
-
Bloating or a tummy that seems to be getting larger
-
Reduced appetite or feeling full very quickly
-
Nausea or vomiting
-
Unexplained weight loss
-
A clear change in bowel habits (constipation, diarrhoea, or alternating)
-
New or persistent indigestion or reflux
-
Marked fatigue that is new for you
Let your GP, oncology team, or lung cancer specialist know if you are dealing with any of these symptoms.
What matters most is the overall pattern. I mean, how it differs from your normal, how long it’s been going on, and what else has changed.
This is important because symptoms on their own can be misleading. The same symptom can mean very different things depending on the context.
If we know how it differs from what is normal for you, we can tell whether this is a genuine new development or part of a long-standing issue like reflux, IBS, or constipation that tends to flare.
How long it has been going on helps us separate problems that are likely to settle on their own from problems that need investigating. A day or two of nausea after a treatment cycle is very different from nausea that is steadily worsening over two or three weeks.
And whether other symptoms have appeared or changed at the same time is often what points us in the right direction. Abdominal discomfort on its own might be constipation. Abdominal discomfort plus fever might suggest infection. Abdominal swelling plus breathlessness might suggest fluid build-up. Pain plus jaundice raises a different set of concerns again.
You are not being asked to diagnose yourself. You are simply giving your team the details that make it much easier to triage properly and act quickly.
Symptoms by common site of spread
Liver
The liver is one of the more common abdominal sites for lung cancer spread.
Possible symptoms include:
-
A dull ache or heaviness under the right ribs
-
Feeling full quickly, nausea, reduced appetite
-
Unexplained weight loss
-
General itching or feeling unwell
Less common, but more urgent symptoms include:
-
Jaundice (yellowing of the eyes or skin)
-
Dark urine and pale stools
A lot of liver involvement is picked up on scans and blood tests before symptoms become dramatic. So if your team mentions “liver lesions”, it does not automatically mean you should feel awful straight away. It just means we need a plan.
Adrenal glands
Adrenal metastases are often silent. People can have them and feel absolutely nothing.
If symptoms occur, they might include:
- Vague flank or back pain
Very rarely, if both adrenal glands are affected and the body cannot produce enough steroid hormone, people can develop adrenal insufficiency. Symptoms can include:
-
Profound fatigue and weakness
-
Dizziness on standing, low blood pressure
-
Nausea, abdominal pain
This is uncommon, but it is important because it is treatable and, if severe, it needs urgent medical attention.
Peritoneum and fluid build-up (ascites)
If cancer involves the lining of the abdomen, fluid can accumulate. This can cause:
-
Increasing abdominal distension or tightness
-
Feeling full quickly
-
Nausea
-
Shortness of breath from pressure pushing up on the diaphragm
-
Swelling in the legs
This is one of those situations where earlier intervention often means easier symptom control. Drainage can help, and there are longer-term options in selected cases.
Abdominal lymph nodes
Enlarged abdominal lymph nodes may cause no symptoms at all.
If they do cause symptoms, they are often vague, usually just a sense of abdominal discomfort or back pain. More severe symptoms are unusual, but significant disease can sometimes contribute to obstruction-type symptoms, which I cover below in the red flags section.
Bowel involvement (rare, but important)
Direct spread to the bowel is not common in lung cancer, but it can happen.
Symptoms to watch for include:
-
Cramping abdominal pain
-
Persistent constipation, or inability to pass wind
-
Vomiting, increasing abdominal swelling
-
Blood in the stool, or black stools
If you have severe pain, a rigid or hard tummy, fever, or you cannot keep fluids down, that needs urgent assessment.
Pancreas (uncommon)
Pancreatic involvement is uncommon, but possible symptoms include:
-
Upper abdominal pain, sometimes radiating through to the back
-
Nausea and weight loss
-
Jaundice (if the bile duct becomes blocked)
Bone spread that feels like abdominal pain
Not all “abdominal” pain is abdominal.
Spread to bones in the spine, ribs, or pelvis can feel like:
-
Deep ache in the back, flank, or pelvis
-
Pain that is worse with movement or at night
If you develop numbness, weakness, or changes in bladder or bowel control, that is an emergency. It can indicate spinal cord compression, and we need to treat that quickly.
Common causes that are not cancer spread but still need treatment
Even in someone with lung cancer, abdominal symptoms are very often caused by problems that are not cancer spread.
Constipation is a big one, particularly if you are taking opioid painkillers, anti-sickness medication, moving less than usual, or are dehydrated. Reflux or gastritis is also common and can be worsened by steroids or stress. Nausea can be a direct treatment side effect from chemotherapy, antibiotics, or painkillers. Viral stomach bugs, gallstones, urinary infections, and kidney stones can all cause convincing abdominal pain and discomfort, too.
It is also important not to miss treatment-related liver irritation, including immunotherapy-related hepatitis. This matters, and it should not be ignored.
This is why it is rarely helpful to self-diagnose based solely on symptoms. The same symptom can have a simple or serious cause. We work it out by looking at the whole picture.
When to seek urgent help
Call your team urgently, seek same-day medical advice, or go to A&E if you have severe or sudden abdominal pain, persistent vomiting, or you cannot keep fluids down, or symptoms that suggest bowel obstruction, such as severe bloating, cramping pain, and not being able to pass stool or wind.
You should also seek urgent help if you develop jaundice, very dark urine and pale stools, fever with abdominal pain (especially during treatment), vomiting blood, black stools, or significant rectal bleeding. New leg weakness, numbness, or changes in bladder or bowel control need emergency assessment, as do severe dizziness, fainting, confusion, or collapse.
While this list is not exactly soothing, it‘s better to be clear. These are the situations where waiting it out can backfire.
How we investigate abdominal symptoms
What we do depends on your symptoms, your current treatment, and what we already know from your scans. Typically, we start with a careful history, including where the pain is, what makes it better or worse, any bowel changes, appetite changes, weight trends, and any recent medication changes. We often do blood tests as well, usually including a full blood count, kidney function, liver tests, and inflammation markers, with additional tests depending on the situation.
Imaging is often the next step. That might be an ultrasound or a CT scan of the abdomen and pelvis, and sometimes an MRI if we need a clearer answer about the liver. If infection or bleeding is part of the picture, urine or stool tests may be useful.
Occasionally, I recommend endoscopy if symptoms point towards a stomach or bowel cause. Sometimes we also need a biopsy to confirm the nature of a lesion, particularly if the result would change the treatment approach.
What treatment and symptom relief can look like
If symptoms are being driven by constipation, reflux, or treatment side effects, we treat those directly, and it can be surprisingly effective and quick. If symptoms relate to metastatic disease, treatment may include systemic therapy such as targeted therapy, immunotherapy, or chemotherapy to control the cancer overall. Radiotherapy can help with painful bone disease or specific problem areas, and procedures like drainage can relieve discomfort if fluid build-up (ascites) is contributing. We also take pain management seriously, tailoring it to the type of pain rather than simply escalating doses, and we often involve dietitians and hydration support to help people stay stronger throughout treatment.
A quick note on specialist supportive care. Involving them is not ‘giving up’. It is us treating symptoms properly so you feel and function better, while cancer treatment continues.
What you can do at home (without becoming your own full-time clinician)
You do not need to monitor everything, but a few simple notes can help your team. You should take note of the following:
-
When symptoms started, and whether they are improving or worsening
-
Bowel movements (especially if constipation is a risk for you)
-
Weight trend over a couple of weeks, if appetite has changed
-
Any fever, vomiting, or inability to keep fluids down
-
Any medication changes, including new painkillers or anti-sickness drugs
And if you are sitting on a symptom because you do not want to be a nuisance, please don’t. This is not nuisance territory. This is exactly what we are here for.
Doing the sensible thing
Abdominal symptoms in someone with lung cancer are common, and many are treatable and not caused by spread. But new, persistent, or worsening symptoms should be assessed early, because if something is changing, we would rather catch it while it is still manageable.
The main thing is not to sit with symptoms in silence, trying to work out what they “must” mean. You are not expected to diagnose yourself. You are expected to notice what has changed and tell your team. In most cases, the answer is something fixable, like constipation, reflux, infection, or a medication side effect, and dealing with it promptly can make a real difference to how you feel day to day. And if scans do show progression, earlier assessment gives us more options, more breathing space, and usually a smoother path to getting symptoms back under control.
About Dr. James Wilson
Dr. James Wilson is a consultant oncologist specialising in lung cancer and advanced radiotherapy. Based in Central London, he works full-time in private practice, aiming to provide rapid diagnosis, clear plans, and calm, practical guidance when time matters.