What Is Stereotactic Radiotherapy and How Does It Work?
When most people hear the word “radiotherapy”, they picture weeks of daily hospital visits. Tiredness builds up. Life put on hold. For a long time, that was an accurate picture.

Jump to:
Stereotactic radiotherapy is different. It's one of the most significant developments in radiation oncology over the past two decades, and I still think it's underexplained to patients who might genuinely benefit from it.
Here's a straightforward account of what it is, how it works, and who it might be right for.
What Is Stereotactic Radiotherapy?
Stereotactic radiotherapy, commonly known as SABR (Stereotactic Ablative Radiotherapy), is a form of precision radiation treatment. It's sometimes called SBRT, or Stereotactic Body Radiotherapy. The two terms refer to essentially the same approach, and you'll often see them used interchangeably.
The word "ablative" is an important term to remember. It means that the dose is high enough not just to slow tumour growth, but to destroy tumour cells directly. This is quite different from conventional radiotherapy, which typically delivers lower doses over a long course to gradually damage cancerous tissue.
With SABR, the radiation is shaped with extraordinary precision to match the exact dimensions of a tumour. Rather than a broad beam passing through a wide area of tissue, multiple beams converge from different angles onto a single point, the tumour itself, whilst the surrounding healthy tissue receives only a fraction of the total dose.
The result is a treatment that can be delivered in as few as one to five sessions, rather than the four to six weeks of daily treatment that conventional radiotherapy often requires.
How It Actually Works
The precision SABR relies on starts well before the patient walks into the treatment room. It begins with detailed imaging, usually a combination of CT and PET scans, to map the tumour's exact position and size down to the millimetre. That information is used to design a treatment plan that shapes the radiation dose to fit the tumour's contours precisely.
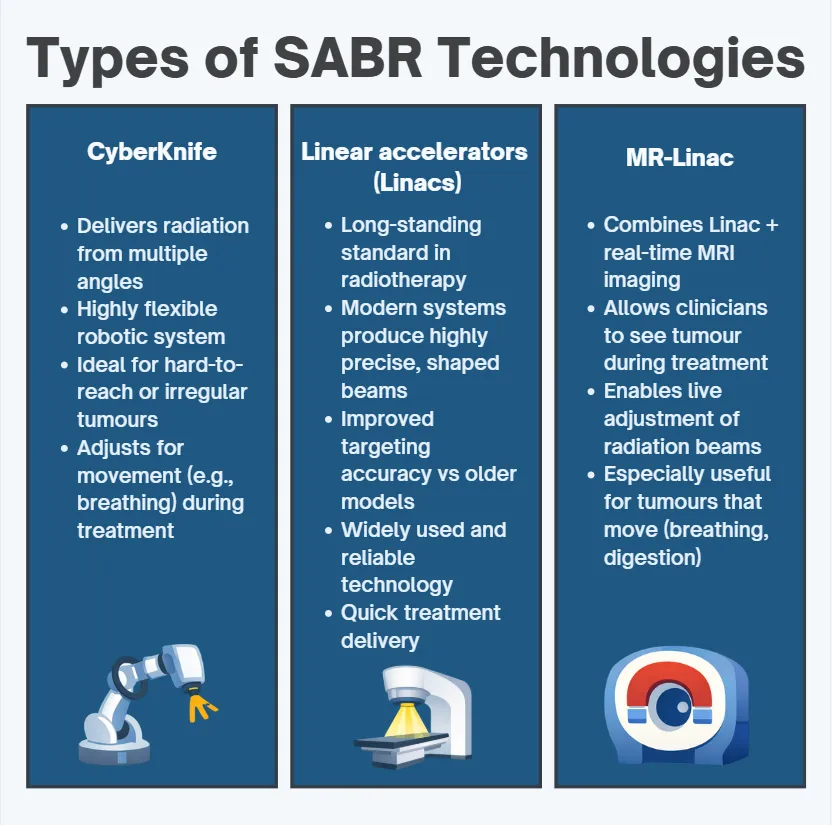
Three main technologies are used to deliver SABR, and which one is used depends on the tumour's location and complexity.
CyberKnife uses a robotic arm to deliver radiation from multiple angles with a degree of flexibility that makes it particularly well-suited to tumours in awkward or hard-to-reach locations. It can also account for slight movement, such as breathing, during treatment.
Linear accelerators (Linacs) have been used in radiotherapy for decades for quick delivery of treatment. Still, modern versions can produce highly precise, shaped beams that can target tumours with far greater accuracy than earlier models.
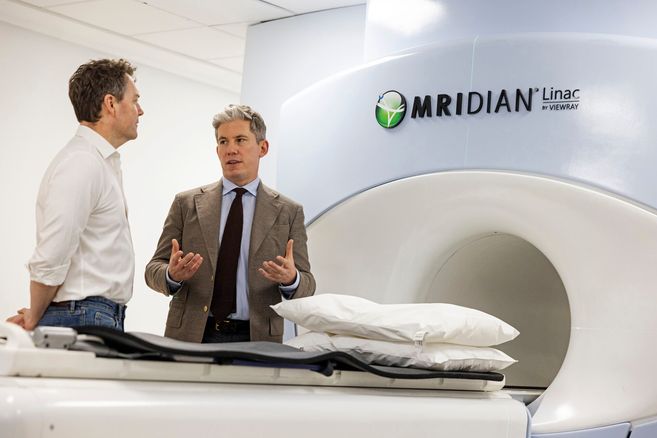
MR-Linac is, I think, one of the more exciting developments in this space. It combines a linear accelerator with real-time MRI imaging, so the clinician can see the tumour during treatment and adjust the beam accordingly. For tumours that move slightly with breathing or digestion, that level of real-time guidance matters.
A session itself is, for most patients, is unremarkable in the best possible way. It's painless. It feels much like having an X-ray. Depending on the technology being used and the complexity of the treatment plan, a session might last anywhere from fifteen minutes to around an hour. Patients go home the same day and return to their normal routine fairly quickly.
What Conditions Can SABR Treat?
This is where it gets genuinely interesting, because the range of situations where SABR is useful has expanded considerably.
Early-stage lung cancer is perhaps the most well-established use. For patients with small, localised tumours who aren't suitable for surgery, either because of age, fitness, or other health conditions, SABR can achieve cure rates comparable to an operation. That's a meaningful option.
Oligometastatic disease is where I spend a lot of my clinical thinking. Oligometastatic means cancer that has spread to a small number of specific sites, typically one to five. Rather than treating the whole body with systemic therapy, SABR can target each of those spots directly. The aim is to control or eradicate them, rather than simply slow them down. The SABR-COMET trial, an important international study, showed that some patients with oligometastatic cancer remained disease-free for more than five years after treatment. That's not something we could have said confidently a decade ago.
Oligoprogressive disease is a related but slightly different situation. This is where a patient is on a drug that's working well overall, keeping most of the cancer under control, but one or two spots start to grow through it. In that case, SABR can be used to treat just those progressing areas whilst the effective drug continues. It can mean staying on a treatment that's working rather than moving on to a more aggressive regimen before it's necessary.
Tumours near critical structures are another area where SABR's precision becomes particularly valuable. Cancers close to the heart, spine, liver, major airways, or brain can be extremely difficult to treat surgically without significant risk. SABR's ability to concentrate the dose on the tumour whilst sparing adjacent tissue makes it a realistic option in situations where surgery wouldn't be appropriate.
The cancer types where SABR is used include lung, breast, prostate, colorectal, and melanoma, amongst others.
What Patients Can Expect
Before treatment begins, there's a planning phase. You'll have scans, the treatment team will map your tumour, and a plan will be designed specifically for you. This typically takes a number of days.
The treatment sessions themselves are usually short and straightforward. You'll be positioned carefully, the machine will do its work, and you'll be free to leave. Most people find it far less disruptive than they anticipated.
Side effects, for most patients, are mild and short-lived. Fatigue is the most common one. Depending on the area being treated, there may be some mild skin irritation, a slight cough for lung treatments, or brief headaches for brain treatments. Serious side effects, which are classified as grade 3 to 5 toxicity, affect fewer than two in every hundred patients. That's a reassuring figure, though it's worth discussing your specific situation in detail with your oncologist.
One of the practical advantages of SABR is that the recovery time is minimal. Most patients are back to their normal routines within a day or two, not weeks.
Why It Can Make a Real Difference for Lung Cancer
There's a shift in how we think about lung cancer that's been building for some years now, and SABR is part of it.
Lung cancer, and its treatment, isn't always what it used to be. With better drug therapies, particularly targeted treatments for patients with specific mutations, like EGFR or ALK, and immunotherapy for others, more patients are living longer with advanced disease. The question increasingly isn't just "can we treat this?" but "how do we keep this under control for as long as possible, without making daily life miserable in the process?"
SABR fits into that picture in a few ways. For early-stage lung cancer, it offers a genuine alternative to surgery in patients who can't tolerate an operation, with cure rates that hold up well against surgical outcomes. For advanced lung cancer that has spread to a small number of sites, it can target each of those areas directly whilst systemic treatment continues in the background.
Where I find it particularly useful is in oligoprogressive lung cancer. A patient might be doing well on a targeted therapy, most of their disease controlled, but one spot in the liver or a lymph node starts moving. Rather than abandoning a treatment that's working elsewhere, SABR can deal with that single progressing lesion. It buys time. It keeps an effective drug going a bit longer. That matters.
In my own practice, tumour control rates for lung lesions treated with SABR are over 90%. For carefully selected patients with oligometastatic disease, that figure can approach 95%. These aren't numbers I quote to impress. They reflect the importance of choosing the right patients for the right treatment.
SABR also has a practical quality-of-life advantage that I think gets underappreciated. Because treatment is delivered in just a handful of sessions, patients aren't spending weeks in the hospital. They're not dealing with the cumulative fatigue of a long radiotherapy course on top of everything else. For someone already managing a lung cancer diagnosis, that's not a small thing.
Is SABR Right for You?
This depends on a number of things, and it's honestly not a question that can be answered without a proper consultation with an oncology specialist and a look at your imaging.
What I would say is that SABR works best when it's considered as part of a full picture. I'm trained in both drug therapies and radiation oncology, and I think that breadth matters. A patient considering SABR should be assessed by someone who can weigh up all the options, not just the ones they specialise in.
If you're wondering whether SABR might be relevant to your situation, a consultation is the right starting point in a private setting, which can usually happen within 48 hours. You don't need a GP referral, and if you have questions before then, we're happy to talk through them.
There are no guarantees in oncology, and I'd never pretend otherwise. But for the right patient, stereotactic radiotherapy is a genuinely powerful tool. It's worth knowing about.
About Dr James Wilson
Dr James Wilson is a consultant oncologist in London specializing in lung cancer and advanced radiotherapy. He works full-time in private practice, focusing on fast diagnosis, well-structured treatment plans, and clear, reassuring guidance, particularly when timely decisions are essential. He is dedicated to delivering the highest standard of care, combining leading-edge technology with extensive clinical experience to achieve the best possible results.
If you’ve been diagnosed with oligometastatic disease, specialist stereotactic radiotherapy may offer a meaningful improvement in your outcome. Get in touch today to discuss your diagnosis and learn how advanced treatment options can be tailored to your individual needs.