How Fast Does Small Cell Lung Cancer Spread?
This is usually not an abstract question. People ask it because something has just happened: A scan. A biopsy. A sentence that included the words “small cell”.


Jump to:
- The short answer
- What makes small cell lung cancer different
- How doctors describe the spread in small cell lung cancer
- How quickly can it spread?
- Where small cell lung cancer commonly spreads
- Symptoms that can suggest the spread
- How spread is assessed
- If it spreads quickly, can treatment still work?
- Why timing matters, but panic does not help
- Getting rapid clarity and a plan
- About Dr. James Wilson
Small cell lung cancer behaves differently from other lung cancers. That difference is the reason this question comes up so often, and why the answers need to be very clear, not a runaround given by a healthcare provider.
The short answer
Small cell lung cancer tends to spread faster than most other types of lung cancer.
This is the reason why it is often described as aggressive. Not to be dramatic, but to reflect how quickly it can grow and move beyond the lungs if left untreated.
Fast spread does not mean there are no treatment options. It does mean that timing and coordination matter.
What makes small cell lung cancer different
Small cell lung cancer has a distinct biological behaviour. The cancer cells divide rapidly and are more likely to travel early through lymphatic channels and the bloodstream.
As a result, many people are diagnosed after the cancer has already spread, even if symptoms have only been present for a short time.
This is different from non-small cell lung cancer, which can grow more slowly and may stay confined to the lung for longer.
How doctors describe the spread in small cell lung cancer
Rather than using a complex staging system, small cell lung cancer is usually described in two broad categories:
Limited-stage disease means the cancer is confined to one side of the chest and can be treated within a single radiotherapy field. At this stage, it is typically localised to the lung and nearby lymph nodes, without spreading to distant organs. Because of this, treatment often aims to control the disease more aggressively, usually combining chemotherapy and radiotherapy. Early identification at this stage can improve the likelihood of a better treatment response.
Extensive-stage disease means the cancer has spread beyond that area, either to the other lung or to distant parts of the body. This may include spread to organs such as the liver, bones, brain, or adrenal glands. In this stage, treatment focuses more on controlling the disease, relieving symptoms, and maintaining quality of life. Systemic therapies such as chemotherapy, immunotherapy, or targeted treatments are commonly used to manage the condition.
The wording can feel misleading. “Limited” does not mean minor, and “extensive” does not mean untreatable. It is simply a practical way of guiding treatment decisions. An oncology specialist would be the best person to ask for more details about this type of cancer.
How quickly can it spread?
There is no single timeline that applies to everyone.
In general terms, small cell lung cancer can progress over weeks to months rather than years. Symptoms may evolve relatively quickly, and scans taken a short time apart can sometimes look noticeably different.
That said, not everyone experiences the same pace of disease. Overall health, tumour biology, and the timing of treatment all influence what happens next.
The key point is this: Once small cell lung cancer is suspected, investigations and treatment planning usually move promptly.
Where small cell lung cancer commonly spreads
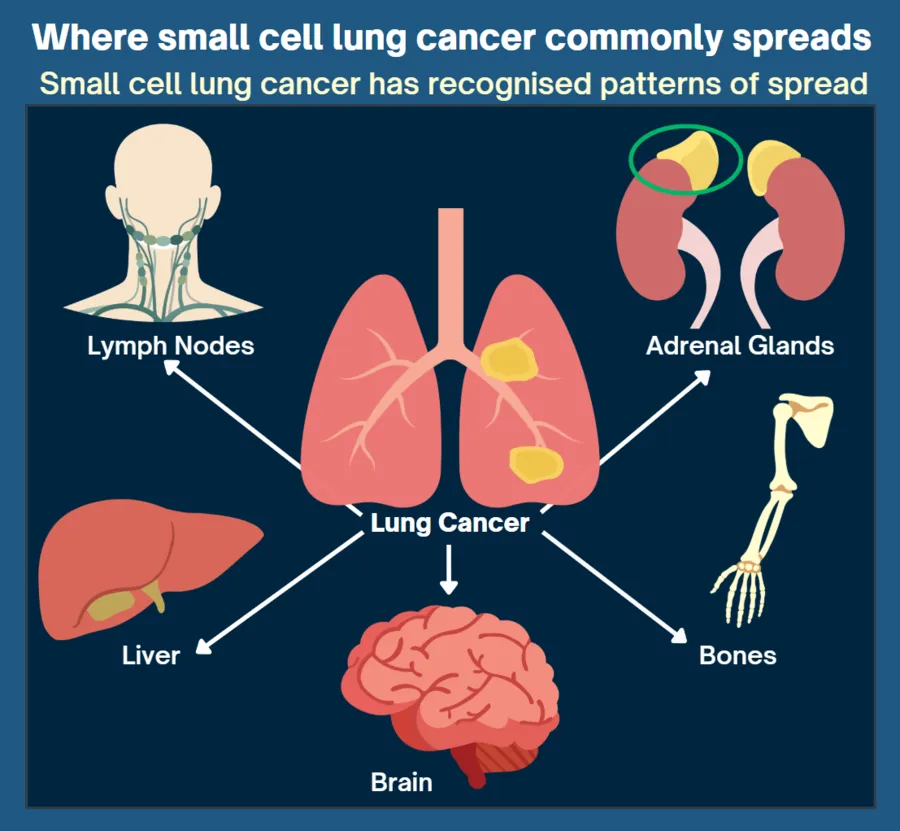
Small cell lung cancer has recognised patterns of spread. Common sites include:
-
Lymph nodes, particularly within the chest
-
Liver
-
Brain
-
Bones
-
Adrenal glands
Brain involvement is especially relevant in small cell lung cancer, which is why brain imaging is often done early, even if there are no neurological symptoms.
Symptoms that can suggest the spread
Symptoms depend on where the cancer is affecting the body. Some are general and non-specific, such as:
-
Increasing fatigue
-
Unintended weight loss
-
Reduced appetite
Others relate more clearly to particular areas:
-
Headaches, balance problems, or confusion if the brain is involved
-
Bone or back pain if bones are affected
-
Abdominal discomfort or jaundice if the liver is involved
Symptoms help guide investigations. They are not used on their own to determine the stage of the cancer.
How spread is assessed
Accurate staging is essential before treatment begins.
This usually involves a combination of imaging, which may include:
-
CT scans of the chest and abdomen
-
PET-CT to assess disease activity throughout the body
-
MRI of the brain
These tests are typically organised quickly once small cell lung cancer is suspected, because treatment decisions depend on having the full picture.
If it spreads quickly, can treatment still work?
There’s an important nuance here.
Although small cell lung cancer spreads quickly, it often responds well initially to treatment. Chemotherapy, often combined with radiotherapy or immunotherapy depending on stage, can shrink the disease rapidly and improve symptoms.
Response and cure are not the same thing, and it is important to be honest about that. But an early response can be meaningful, both for symptom control and quality of life.
Why timing matters, but panic does not help
Speed matters in small cell lung cancer, but panic rarely helps anyone make good decisions.
What helps is prompt assessment, a clear explanation, and a coordinated plan. Most delays happen not because people waited too long, but because the pathway felt fragmented or unclear.
Getting the right information early makes a real difference.
Getting rapid clarity and a plan
Some people are managed entirely through NHS pathways. Others seek an additional specialist opinion to clarify staging or treatment options more quickly.
In my practice, patients can access consultant-led assessment and coordinated investigations when appropriate. Private input can work alongside NHS care, not instead of it.
About Dr. James Wilson
Dr. James Wilson is a consultant oncologist specialising in lung cancer and advanced radiotherapy. Based in Central London, he works full-time in private practice, helping patients with timely diagnosis, clear treatment plans, and calm, practical support, especially when decisions need to be made quickly.