Benefits of Proton Beam Therapy For Lung Cancer
Radiotherapy has been part of lung cancer treatment for a long time. For most of that time, the challenge has been the same. How do you deliver enough radiation to destroy a tumour without causing too much damage to the healthy tissue around it?

Jump to:
- What is radiotherapy, and why does precision matter?
- What is proton beam therapy?
- What does treatment involve?
- What sets proton beam therapy apart
- Greater precision
- Reduced dose to the heart
- Reduced dose to the lungs
- Reduced dose to the oesophagus
- Fewer and less severe side effects
- Suitable for tumours in difficult locations
- Re-irradiation
- When curative treatment has been ruled out
- How proton beam therapy compares to other radiotherapy options
- Who is most likely to benefit?
- An honest note on proton beam therapy
- What is the bottom line?
- About Dr. James Wilson
In the chest, that challenge is especially difficult. The lungs, heart, oesophagus, and spinal cord all sit close together. There isn’t much room for error.
Proton beam therapy changes the equation. It does not do anything that conventional radiotherapy cannot, in terms of its basic purpose. But it does it with a level of precision that was not widely available until relatively recently. For the right patient, that precision can make a meaningful difference.
What is radiotherapy, and why does precision matter?
Radiotherapy works by targeting cancer cells with high-energy beams. The radiation damages the DNA inside those cells, so they cannot divide and grow. Over the course of treatment, the aim is to destroy the tumour.
The complication is that the beams also pass through healthy tissue on the way. In the case of conventional X-ray radiotherapy, they continue delivering a dose after the target. That exit dose is unavoidable with standard radiotherapy. Managing it is part of the planning process, and modern radiotherapy does this well.
But in the chest, even a well-planned conventional treatment involves some of the dose reaching the heart, the healthy lung, and other structures nearby. That can have consequences. The goal with any advance in radiotherapy technology is to keep reducing that collateral dose while maintaining or improving control of the tumour.
What is proton beam therapy?
Proton beam therapy is a form of radiotherapy that uses protons rather than X-rays. The key difference lies in something called the Bragg peak. When protons travel through tissue, they slow down gradually, then release the vast majority of their energy at a very specific depth, and then stop.
Conventional X-rays do not behave that way. They deposit the dose throughout the tissue they pass through, including beyond the target.
The practical result is this. Proton beam therapy delivers a concentrated dose to the tumour and very little to the surrounding tissue. The exit dose, which is a built-in limitation of conventional radiotherapy, is largely eliminated. In a part of the body as complex as the chest, that is a significant advantage.
What does treatment involve?
Before treatment begins, a detailed planning process takes place. The team uses CT and sometimes other imaging to map the tumour precisely, so the proton beams can be shaped and directed to match it.
Treatment itself is delivered in sessions, typically over several weeks. The sessions are not painful. Patients lie still while the beams are directed at the target area. The number of sessions depends on the individual treatment plan.
What sets proton beam therapy apart
Greater precision
Proton beam therapy can be shaped and directed to match the exact dimensions and position of the tumour. That degree of precision is particularly valuable in the chest, where the tumour may be sitting close to the heart, oesophagus, spinal cord, or major blood vessels.
For centrally located tumours, this is not a minor refinement. It is often the difference between a treatment being safely deliverable or not.
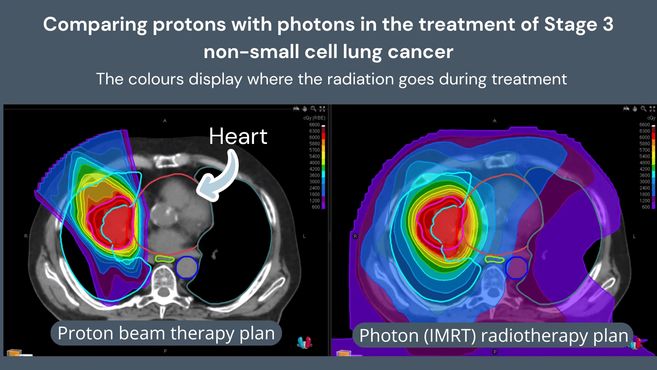
Reduced dose to the heart
Radiation to the heart is one of the significant concerns with conventional chest radiotherapy. Long-term cardiac effects, including an increased risk of heart disease, are a recognised consequence of chest radiotherapy, particularly when treating tumours on the left side.
Proton beam therapy substantially reduces the dose reaching the heart. For patients who are otherwise well and have many years ahead of them, that matters.
Reduced dose to the lungs
Radiation pneumonitis, which is inflammation of the lung tissue caused by radiotherapy, is a known complication of chest treatment. It can range from mild and manageable to serious. Reducing the dose to healthy lung tissue lowers that risk considerably.
For patients who already have reduced lung function, whether from COPD, previous lung disease, or prior surgery, this is especially important. There is less reserve to lose.
Reduced dose to the oesophagus
Inflammation of the oesophagus during and after treatment is a common side effect of conventional chest radiotherapy. It can make eating and swallowing uncomfortable, sometimes significantly so.
Proton beam therapy reduces the dose to the oesophagus, which typically means less inflammation and a more manageable experience during treatment.
Fewer and less severe side effects
The cumulative effect of reducing dose to healthy tissue is that patients often tolerate treatment better overall. There is less fatigue in some cases. Less acute inflammation. Lower risk of long-term organ damage.
That does not mean proton beam therapy is free from side effects. It is still radiotherapy, and it still requires careful planning and monitoring. But the overall profile is generally more favourable.
Suitable for tumours in difficult locations
Some tumours sit in positions where delivering conventional radiotherapy at the required dose would carry unacceptable risk to the surrounding structures. Centrally located tumours, those near the main airways or major blood vessels, are a clear example.
Proton beam therapy can sometimes make treatment feasible in situations where conventional radiotherapy would be limited, including patients with complex anatomy and those who have already received radiotherapy to the same area.
Re-irradiation
If a patient has already received radiotherapy and the disease has recurred or progressed in the same region, re-treating with conventional radiotherapy may not be possible. The surrounding tissue has already received its safe lifetime dose.
Proton beam therapy, because of its precision and reduced exit dose, can sometimes make re-irradiation possible. For patients in that situation, it may open up options that would otherwise not exist.
When curative treatment has been ruled out
Some patients are told, based on the location or complexity of their tumour, that surgery is not an option and that curative-intent treatment is not feasible.
That assessment is sometimes correct. But not always. Some patients in complex situations, who would not be candidates for conventional curative radiotherapy, can still be considered for proton beam therapy. It is always worth a review from an oncology consultant before concluding that radical treatment is off the table.
How proton beam therapy compares to other radiotherapy options
There are several advanced radiotherapy techniques used in lung cancer treatment. They are not competing with each other. They are different tools, and the right choice depends on the individual case.
| Treatment | Key feature | Often best suited to |
| Conventional radiotherapy | Established, widely available | Many lung cancers across all stages |
| SABR | Very high dose per session, highly targeted, fewer sessions | Early-stage and oligometastatic disease |
| CyberKnife | Robotic delivery, real-time imaging | Smaller, well-defined tumours |
| MR Linac | MRI-guided, adapts to tumour position in real time | Tumours close to sensitive structures |
| Proton beam therapy | Minimal exit dose, maximum sparing of surrounding organs | Complex or central tumours, re-irradiation, reduced lung reserve |
A patient being assessed for radiotherapy will usually have a discussion with their oncology specialist about which approach is most appropriate for their situation. In some cases, more than one technique might be considered. In others, one approach is clearly better suited.
Who is most likely to benefit?
Proton beam therapy is not the right treatment for every patient with lung cancer. But for certain groups, the advantages are substantial.
It is worth considering for patients with centrally located tumours, close to the heart, oesophagus, major airways, or spinal cord. It is also particularly relevant for patients where the dose to the heart or healthy lung needs to be kept especially low, including those with existing heart disease or reduced lung function. Patients with stage 1 to 3 non-small cell lung cancer being considered for radical, curative-intent treatment are another important group.
Beyond that, it is especially worth exploring for anyone who has already received radiotherapy to the chest and may need treatment again, and for patients who have been told that surgery is not an option and want to understand what alternatives exist.
An honest note on proton beam therapy
Proton beam therapy is an increasingly well-supported option in lung cancer treatment, but it is not suitable for everyone and does not guarantee a specific outcome. Whether it is appropriate depends on a specialist review of the full clinical picture, including the cancer’s type, stage, location, previous treatments, and overall health.
In the right circumstances, it can offer more precise treatment, fewer side effects, and, for some patients, options that might not otherwise be available. If you would like to explore whether proton beam therapy could be relevant to you, a specialist consultation is the best first step.
What is the bottom line?
Proton beam therapy represents a meaningful step forward in how we treat lung cancer with radiotherapy. For the right patient, it means a more targeted treatment, a better side effect profile, and in some cases, options that simply would not be available with conventional approaches.
The most important first step, if you are trying to work out whether it applies to you, is getting a proper specialist review. Not a Google rabbit hole at midnight. An actual conversation with someone who can look at the full picture and give you a straight answer.
About Dr. James Wilson
Dr. James Wilson is a consultant oncologist specialising in lung cancer and advanced radiotherapy. Practising full-time in Central London, he focuses on delivering prompt diagnoses, straightforward treatment strategies, and steady, practical support for patients when decisions need to be made quickly.